There is no shortage of people who report of soreness and stiffness in their upper trapezius (UT) region. The automatic assumption that many clinicians make is that if it is sore and the patient perceives it is stiff, well it then must be stiff! So the obvious solution is to somehow “release & stretch” the UT muscle in order to loosen it.
These two separate studies used a relatively new technology called shear wave elastography, to compare the stiffness of the neck extensors between women with chronic neck pain and asymptomatic controls during multiple tasks.
Conclusion: Neck muscle stiffness was NOT different between those with neck pain and asymptomatic controls.
“…severity of pain and disability did not correlate to stiffness of these muscles in patient”–Tas et al 2018
Clinical relevance #1: The clinical assumption that patient perceived neck stiffness corresponds to objective muscle stiffness must be questioned
Clinical relevance #2: Therapies that aim to reduce neck muscle stiffness also need to be questioned
Personal comment: I am not against the use of various soft-tissue techniques, needling, or cupping that anecdotally make patients feel better. I am quoting these 2 studies not to stop us from practicing these therapeutic interventions but to appreciate that their effectiveness is likely a result of neuromodulation of pain rather than actual “loosening of the muscles”.
I am also always amazed when clinicians are so quick to blame the trapezius muscle when there is discomfort in the region. I may be wrong, but I think we should be blaming the trapezius muscle a lot less often.
Here is a simple test. On your next patient who presents with pain along their UT, resist shoulder shrugging and see if it reproduces their pain. I will put a lot of money down that it will not.
Think of it, if you had an injured or sensitive hamstring muscle, resisted knee flexion would obviously reproduce their hamstring pain.
So what can we conclude when a patient reports of pain along their upper trapezius region but resisted shoulder shrugs do not reproduce their neck pain? Perhaps it is referred pain? I’m still honestly not sure… we got so much to learn!
If the UT symptoms is not related to an acute trauma (e.g. MVA), if neural tissue sensitivity has been rule out (with neurodynamic tests) and I cannot find a definite directional preference (with repeated movements), I consider cupping.
By cupping I am referring to Tissue Distraction Release (TDR) with movement. I still avoid telling my patients that TDR technique helps “loosen muscles up” cause that’s likely not true. I explain to them that I am cupping in order to give the skin and the nerves in the region a different type of stimulation which sometimes helps reduce the sensitivity in the region.
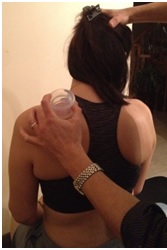
I used to distribute the TDR silicone cups but I stopped as they are now sold wherever acupuncture needles are sold. If anyone needs the large TDR cups, I have a few left.
References: 1. Taş S et al Neck Muscle Stiffness in Participants With and Without Chronic Neck Pain: A Shear-Wave Elastography Study. J Manipulative Physiol Ther. 2018 Sep;41(7):580-588.
-
Dieterich AV et al Neck Muscle Stiffness Measured With Shear Wave Elastography in Women With Chronic Nonspecific Neck Pain. J Orthop Sports Phys Ther. 2020 Apr;50(4):179-188.

